📞 +44 0161 495 7011 (9am - 5pm ᐧ Mon - Fri)
Urinary incontinence is defined as the unintentional passing of urine. It is a remarkably common condition, thought to affect millions of individuals across the UK. While often associated with the ageing process, it is not an inevitable consequence of getting older. The condition can range from small, occasional leaks when coughing or sneezing to a complete inability to control the bladder, which can significantly impact a person’s quality of life, mental health, and social confidence.
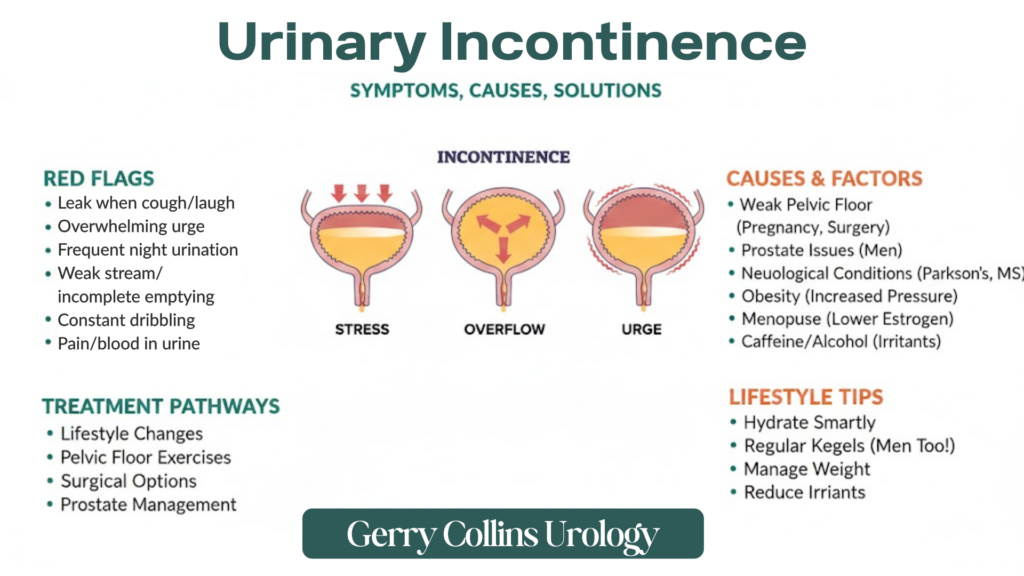
In urological practice, we categorise incontinence into several distinct types. Stress incontinence occurs when the bladder is under sudden physical pressure. Urge incontinence, often linked to an “overactive bladder,” involves a sudden, intense need to pass urine. Overflow incontinence occurs when the bladder cannot empty fully, leading to frequent dribbling, while total incontinence refers to a complete lack of storage capacity. Understanding these distinctions is the first step toward effective management.
The Red Flags
Many people tolerate bladder leaks for years before seeking help, often due to embarrassment. However, certain symptoms require a structured clinical evaluation to rule out underlying issues. You should consult a specialist if you experience:
- Sudden, involuntary leakage when you laugh, cough, or exercise.
- An overwhelming, “must-go-now” urge that you cannot suppress.
- Waking up multiple times during the night to urinate (nocturia).
- A weak urinary stream or a feeling that your bladder is never quite empty.
- Constant dribbling of urine throughout the day.
- Pain during urination or the presence of blood in the urine (haematuria).

Mr. Collins Approach
While many clinics may offer a generic pathway, for men, this often involves a deep analysis of prostate health, as an enlarged prostate (BPH) is a frequent driver of overflow and urge symptoms.
For all patients, Mr Collins integrates advanced diagnostics with a nuanced understanding of pelvic floor biology for a tailored treatment plan.
Causes & Risk Factors
Incontinence is often a multi-factorial issue where biology, lifestyle, and medical history intersect. Common causes include:
Treatment pathways
Treatment is tailored to the specific type and severity of the incontinence, moving from conservative measures to more advanced interventions.
Medical and Conservative Pathways:
- Lifestyle Modification: Identifying and reducing bladder irritants such as caffeine, alongside weight management.
- Bladder Training: Learning to increase the time between urges to improve bladder capacity.
- Pelvic Floor Muscle Training (PFMT): Structured exercises to strengthen the muscles that support the bladder and urethra.
- Medication: Anticholinergics or Mirabegron can be highly effective in calming an overactive bladder.
Surgical and Procedural Pathways:
- Sling Procedures: For stress incontinence, a small ribbon of material is used to support the urethra.
- Botulinum Toxin (Botox): Injections into the bladder wall can relax overactive muscles for those with severe urge incontinence.
- Sacral Nerve Stimulation (SNS): A small device is implanted to regulate the nerve signals to the bladder.
- Prostate Management: If the cause is an obstruction, addressing the prostate size can often resolve the urinary leakage.
Lifestyle tips
While some risk factors are outside of your control, you can take proactive steps to maintain bladder health:
- Hydrate Smartly: Do not restrict fluids too severely, as concentrated urine can irritate the bladder. Aim for steady intake, but reduce fluids two hours before bed.
- Pelvic Floor Strength: Regular “Kegel” exercises are not just for women: they are vital for men, especially those undergoing prostate treatment.
- Manage Your Weight: Reducing even a small amount of weight can significantly decrease the pressure on your pelvic floor.
- Watch the Irritants: If you notice leaks after drinking coffee, tea, or fizzy drinks, try switching to decaffeinated versions or water.
FAQs
No. While it becomes more common with age, it is a medical condition that can and should be treated. You do not have to “just live with it.”
Counter-intuitively, drinking too little can make the problem worse. Dehydration leads to concentrated urine, which irritates the bladder lining and increases urgency. Focus on the timing and type of fluids instead.
It is less common in men than in women, but it often occurs following certain types of prostate surgery. Specialist assessment is required to determine the best




