📞 +44 0161 495 7011 (9am - 5pm ᐧ Mon - Fri)
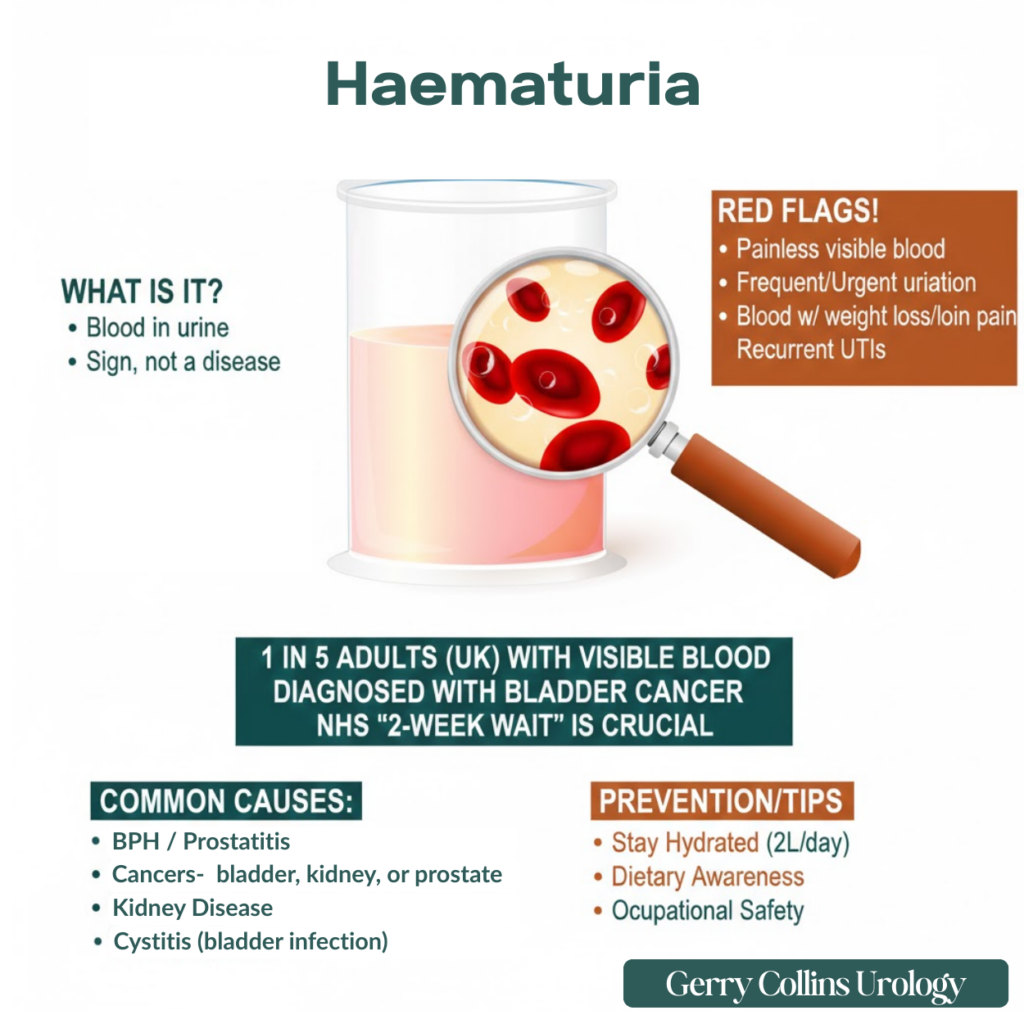
Discovering blood in your urine, a condition known medically as haematuria, can be a distressing experience. While the sight of red or pink-tinted urine often causes immediate concern, it is important to understand that haematuria is a clinical sign rather than a disease in itself. It serves as a biological signal that requires a structured, diagnostic investigation.
In the UK, haematuria is classified into two types: visible (macroscopic), which you can see with the naked eye, and non-visible (microscopic), which is detected via a dipstick test or laboratory analysis.
Did you know:
In the UK, clinical data suggest that approximately 1 in 5 adults who present with visible blood in their urine are subsequently diagnosed with bladder cancer. This highlights the vital importance of the “2-week wait” fast-track referral system used by the NHS to ensure early diagnosis and better long-term outcomes.
The Red Flags
Most episodes of haematuria are not associated with pain, but “painless haematuria” is often the most significant clinical red flag for urological malignancy. You should seek an urgent consultation if you notice:
- Visible blood in the urine, even if it only happens once and then disappears.
- Blood in the urine in the absence of pain or typical infection symptoms, like burning.
- A persistent need to urinate frequently or urgently.
- Blood in the urine, coupled with unexplained weight loss or persistent pain in the sides (loin pain).
- Recurrent urinary tract infections that do not fully clear after a course of antibiotics.

Mr Gerry’s Approach
In an era of rapid, sometimes impersonal medicine, Mr Collins believes the most strategic advantage a patient has is a surgeon who listens. He utilises advanced diagnostics, from high-resolution imaging to flexible cystoscopy, providing a calm, analytical environment where decisions are never rushed, and every patient receives a bespoke management plan.
Causes & Risk Factors
There are various reasons why blood may appear in the urinary tract. These are generally categorised into inflammatory, mechanical, or malignant causes:
Treatment pathways
The pathway to resolving haematuria begins with a structured evaluation, often involving blood tests, a physical examination, and imaging.
Medical & Diagnostic Pathways:
- Flexible Cystoscopy: This is the gold standard for investigating the bladder. A small, flexible telescope is used to inspect the bladder lining under local anaesthetic. It is a quick procedure that provides immediate answers.
- Radiological Imaging: CT scans or ultrasounds are used to visualise the kidneys and ureters to ensure there are no stones or tumours higher up in the system.
- Antibiotics: If an infection is identified as the cause, a targeted course of antibiotics is usually sufficient.
Surgical Pathways:
- TURBT: If a bladder tumour is identified during a cystoscopy, a procedure called Transurethral Resection of Bladder Tumour (TURBT) is performed to remove the growth and provide a precise diagnosis.
- Stone Management: For kidney or bladder stones, laser lithotripsy may be used to break the stones into smaller fragments.
Lifestyle tips to do at home
While some causes of haematuria are beyond your control, you can take steps to protect your urological health:
- Smoking Cessation: Stopping smoking is the single most effective way to reduce your risk of bladder and kidney cancer.
- Hydration: Drinking plenty of water (around 2 litres a day) helps flush the urinary system and reduces the risk of stone formation and infections.
- Dietary Awareness: Be aware that certain foods, such as beetroot or blackberries, and certain medications can temporarily turn urine red, which is harmless but can be mistaken for blood.
- Occupational Safety: If you work in industries involving plastics, rubbers, or dyes, ensure you follow all safety protocols to minimise chemical exposure.
FAQs
Yes. Intermittent bleeding is a common feature of many urological conditions, including tumours. The fact that it stopped does not mean the underlying cause has resolved.
The procedure is performed using a lubricating gel that contains a local anaesthetic. Most patients find it slightly uncomfortable or “odd” rather than painful, and it typically takes less than five minutes.
Yes, “jogger’s haematuria” can occur after very strenuous or long-distance exercise due to minor trauma to the bladder wall. However, this diagnosis can only be made safely after a specialist has excluded other more serious causes.
This is an NHS protocol designed to ensure that anyone with symptoms that could suggest cancer is seen by a specialist within 14 days. Mr Collins works closely within this framework to provide rapid, high-quality assessments for his patients.




