📞 +44 0161 495 7011 (9am - 5pm ᐧ Mon - Fri)
Lower Urinary Tract Symptoms, commonly referred to as LUTS, is an umbrella term used by urologists to describe a range of issues affecting the bladder and the urethra. For many men, these symptoms are often dismissed as an inevitable consequence of ageing, yet they frequently signal underlying changes in the prostate gland or bladder function that require a measured, clinical response.
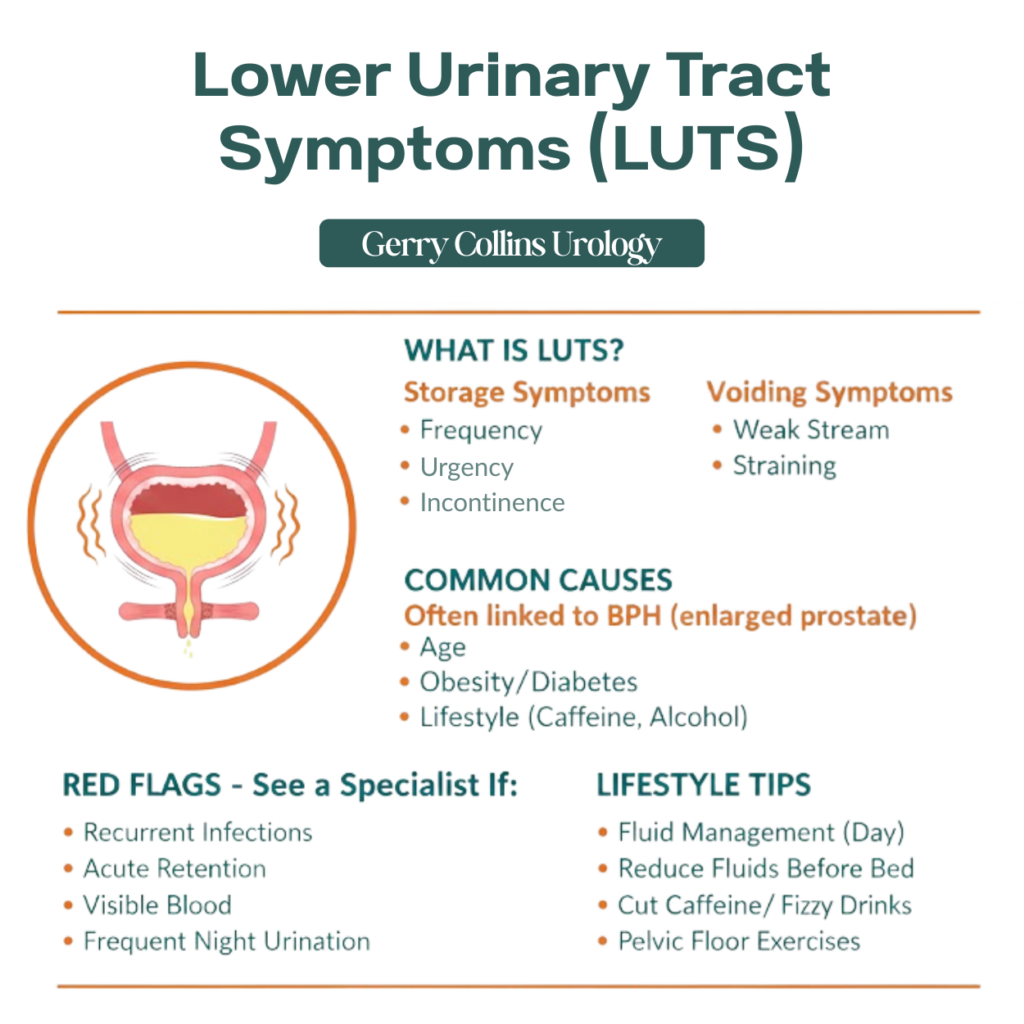
The symptoms are typically categorised into two groups: storage symptoms (how the bladder holds urine) and voiding symptoms (how urine is passed). While often linked to Benign Prostatic Hyperplasia (BPH) or an enlarged prostate, LUTS can also stem from overactive bladder, urethral strictures, bladder cancer or even non-urological issues such as cardiovascular or renal concerns. Understanding the specific biology behind these symptoms is the first step toward reclaiming quality of life.
Did you know:
Lower urinary tract symptoms are remarkably common as men age. In the UK and Europe, approximately 14 percent of men in their 40s experience these symptoms, a figure that rises sharply to 40 percent in men over the age of 60.
Symptoms
While LUTS often develops gradually, certain “red flags” indicate that the bladder or kidneys may be under significant stress. You should seek a specialist consultation if you experience:
- Recurrent Infections: Frequent urinary tract infections (UTIs) which may suggest the bladder is not emptying completely.
- Acute Urinary Retention: A sudden, painful inability to pass any urine at all (this is a medical emergency).
- Visible Haematuria: Seeing blood in your urine, which always requires a structured evaluation.
- Urgency Incontinence: A sudden, uncontrollable need to urinate that results in leakage before reaching a toilet.
- Nocturia: Waking up multiple times a night to urinate, significantly disrupting sleep and metabolic health.

Mr Gerry’s Approach
In many modern clinics, LUTS is met with a reflex prescription or a standard surgical recommendation. Mr. Collins instead utilises advanced diagnostics like Urodynamics, PSA density and Stockholm3 to filter the clinical “noise.”
He believes every treatment plan must be tailored to the individual’s baseline and long-term goals. By analysing the trends in data rather than reacting to a single flow test, he ensures that interventions are measured, strategic, and never rushed.
Causes & Risk Factors
The most frequent cause of LUTS in men is the enlargement of the prostate gland (BPH). As men age, hormonal shifts involve the conversion of testosterone into dihydrotestosterone (DHT), which triggers prostate growth. This growth can squeeze the urethra, forcing the bladder to work harder to expel urine.
Treatment pathways
Treatment is dictated by the severity of the symptoms and the degree of obstruction. Mr. Collins advocates for a risk-stratified approach.
Medical Management:
- Alpha-blockers: These medications (such as Tamsulosin) relax the muscle fibres in the prostate and bladder neck, making it easier to urinate.
- 5-alpha reductase inhibitors: Drugs like Finasteride work by blocking the hormones that cause the prostate to grow, effectively shrinking the gland over six months.
- Combination Therapy: Often the most effective route for mild to moderate symptoms.
Surgical Pathways:
- TURP (Transurethral Resection of the Prostate): The traditional “gold standard” where obstructing tissue is removed to clear the channel.
- Holep and other types of laser.
- Bladder Neck Incision: A strategic option for men with smaller but highly obstructive prostates.
Lifestyle tips to do at home
While you cannot halt the biological clock, you can manage the “noise” of LUTS through proactive habits:
- Fluid Management: Reduce fluid intake two to three hours before bed to manage nocturia, but ensure you drink 1.5 to 2 litres during the day to keep urine diluted.
- Bladder Retraining: If you suffer from frequency, try to gradually increase the time between bathroom visits to “re-educate” the bladder muscle.
- The “Double Void” Technique: After passing urine, wait a few moments and try again to ensure the bladder is fully empty.
- Dietary Adjustments: Reduce caffeine and fizzy drinks, both of which act as significant bladder irritants.
- Pelvic Floor Exercises: Often associated only with women, pelvic floor strength is vital for men to manage “post-micturition dribble” and urgency.
FAQs
No. Most LUTS are caused by benign enlargement (BPH). However, because the symptoms can overlap, Mr Collins performs a thorough assessment, including PSA interpretation and physical examination, to exclude malignancy.
Procedures like TURP carry a high likelihood of “retrograde ejaculation” (where semen enters the bladder during climax). While this does not affect the sensation of orgasm, it is a key consideration for men concerned about fertility. True erectile dysfunction is a less common risk (approx 7-10%) and should be discussed during your consultation.
If symptoms are mild and not distressing, “Watchful Waiting” is a valid pathway. However, if the bladder is constantly struggling against an obstruction, it can lead to permanent thickening of the bladder wall or kidney damage. Early data-led intervention is always safer than waiting for a crisis.
This can be due to reduced bladder capacity or “peripheral oedema.” Suppose your ankles swell during the day, that fluid returns to the bloodstream when you lie down, prompting the kidneys to produce more urine at night. Mr Collins looks at these systemic factors to find the root cause.




