📞 +44 0161 495 7011 (9am - 5pm ᐧ Mon - Fri)
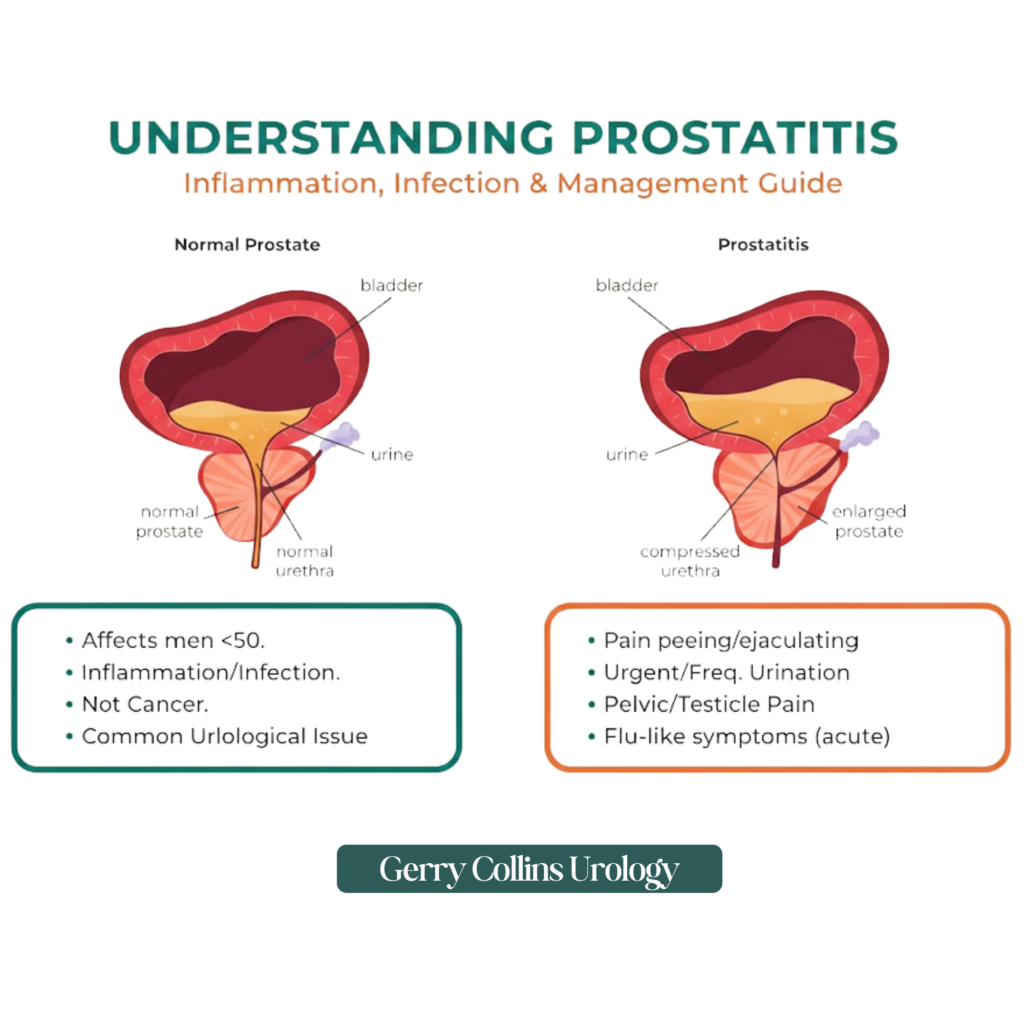
Prostatitis is a term used to describe a set of symptoms caused by the inflammation or infection of the prostate gland. Located just below the bladder, the prostate is a small gland that plays a vital role in male reproductive health. Unlike an enlarged prostate or prostate cancer, which typically affect older men, prostatitis is the most frequent urological issue for men under the age of 50.
While the symptoms can be distressing, it is important to remember that prostatitis is not cancer.
Did you know
Some studies suggest that as many as 10 percent of adult males suffer from prostatitis at some point in their lives. Despite its prevalence, it remains one of the most challenging conditions to diagnose because its symptoms frequently overlap with other urological health issues.
Symptoms
Because the symptoms of prostatitis can be vague or mimic other conditions, it is crucial to seek a specialist opinion if you experience any of the following:
- Pain or a burning sensation when peeing (dysuria).
- Frequent or urgent need to urinate, especially during the night.
- Pain in the perineum (the area between the scrotum and the anus), testicles, or tip of the penis.
- Discomfort or pain during or after ejaculation.
- A feeling that the bladder has not fully emptied.
- Flu-like symptoms such as fever, chills, and lower back pain (typically seen in acute cases).

Mr. Collins Approach
With nearly three decades of experience, Mr. Collins understands that prostatitis can cause significant “noise” in diagnostic data, such as elevated PSA levels.
His approach filters this noise by integrating advanced risk-stratification tools and a deep understanding of prostate biology. He ensures that every patient receives a strategic, measured intervention rather than a rushed or generic treatment plan.
Causes & Risk Factors
The causes of prostatitis are varied and sometimes overlap, making a precise diagnosis essential:
Treatment pathways
Treatment for prostatitis is never “one size fits all.” It is dictated by whether the cause is bacterial or inflammatory.
Medical Pathways:
- Targeted Antibiotics: For bacterial cases, a course of antibiotics is prescribed. While acute cases may resolve in 14 days, chronic bacterial prostatitis may require treatment for four to six weeks to ensure the infection is fully eradicated.
- Alpha-blockers: These medications help relax the muscles where the prostate meets the bladder, improving urine flow and reducing discomfort.
- Pain Management: Specialist analgesics or anti-inflammatories are used to manage pelvic discomfort and swelling.
- The UPOINT Approach: Mr Collins utilises this structured framework to address the urinary, psychosocial, organ-specific, and neurological aspects of the condition simultaneously.
- Acupuncture including moxatherapy
Surgical & Investigative Pathways:
- Flexible Cystoscopy: If symptoms persist, a small telescope may be used to examine the bladder and prostate to rule out other abnormalities.
- Specialised Physiotherapy: For men with chronic pelvic pain syndrome, working with a specialist pelvic floor physiotherapist can help relax overactive muscles.
Lifestyle tips
While you cannot always prevent prostatitis, you can manage the symptoms and reduce the risk of flare-ups through proactive choices:
- Stay Hydrated: Drink plenty of fluids to avoid dehydration and help flush the urinary system.
- Dietary Awareness: Some men find that caffeine, alcohol, and spicy foods irritate the bladder and prostate.
- Warm Baths: “Sitz baths” (soaking the pelvic area in warm water) can help relax pelvic muscles and relieve pain.
- Stress Management: Techniques such as relaxation exercises or mindfulness can be effective, particularly for those whose symptoms are triggered by stress.
- Frequent Ejaculation: Some evidence suggests that regular ejaculation can help clear prostatic secretions and reduce congestion in the gland.
FAQs
No. Prostatitis is a common cause of a high PSA result. Mr Collins uses his 30 years of experience and research into PSA derivatives to interpret these results in context, often avoiding the need for unnecessary biopsies.
In the vast majority of cases, prostatitis is not a sexually transmitted infection and cannot be passed to a partner. However, if an STI is the underlying cause of the inflammation, both partners may need treatment.
While the condition itself can cause painful ejaculation, the treatments for prostatitis are generally focused on restoring normal function. Mr Collins prioritises the preservation of quality of life in every treatment plan.
BPH (Benign Prostatic Hyperplasia) is a non-cancerous enlargement of the prostate that usually affects older men and causes a weak urine stream. Prostatitis is inflammation or infection that often involves pain and can affect men of all ages, particularly those under 50.




