📞 +44 0161 495 7011 (9am - 5pm ᐧ Mon - Fri)
Benign Prostatic Hyperplasia, or BPH, is the medical term for a non-cancerous enlargement of the prostate gland. The prostate is a small gland, usually about the size of a walnut or a satsuma, located just below the bladder. It surrounds the urethra, which is the tube that carries urine from the bladder out of the body. As men age, the prostate often begins to grow.
Because of its location, this enlargement can squeeze the urethra, acting like a bend in a garden hose and making it difficult to pass urine comfortably. It is important to note that BPH is not cancer, nor does it increase your risk of developing prostate cancer, though the two conditions can exist simultaneously.
Did you know:
Approximately 50 percent of men between the ages of 51 and 60 will experience symptoms of BPH, and this figure rises significantly to nearly 90 percent for those over the age of 80.
Symptoms
BPH usually develops slowly, with symptoms that may seem like a minor inconvenience at first but gradually begin to impact your quality of life. You should consult a specialist if you notice:
- A weak or interrupted urinary flow.
- Difficulty starting to urinate or needing to strain.
- A frequent or urgent need to urinate, especially during the night (nocturia).
- A feeling that your bladder has not emptied completely after you have finished.
- Dribbling at the end of the stream.
While these symptoms are common, certain “red flag” situations require urgent medical attention. If you experience a complete inability to pass urine (acute urinary retention), notice blood in your urine (haematuria), or feel significant pain in the lower abdomen or bladder area, you should seek help from a GP or an emergency department immediately.

Mr Gerry’s Approach
Mr Gerry Collins views BPH not as a routine age-related issue, but as a “unique biological puzzle.” With nearly three decades of experience and having conducted significant MD research into BPH and PSA at Edinburgh University and the Mayo Clinic, he looks beyond the raw data of a flow test or a prostate volume measurement to understand how the biology of the gland is affecting the individual.
Causes & Risk Factors
The exact cause of prostate enlargement is not fully understood, but it is heavily linked to the natural ageing process.
Treatment pathways
Management of BPH follows a tiered approach, starting with the least invasive options and moving toward advanced surgical techniques if required.
Medical Pathways:
- Alpha-blockers: Medications like tamsulosin or alfuzosin work by relaxing the muscles in the prostate and bladder neck, making it easier to urinate.
- 5-alpha reductase inhibitors: Drugs such as finasteride or dutasteride can actually shrink the prostate gland by blocking the hormonal changes that cause growth.
- Combined Therapy: In many cases, using both types of medication provides the most effective relief for moderate symptoms.
Surgical & Minimally Invasive Pathways:
For those who do not find relief with medication, Mr Collins offers advanced interventions:
- Rezum (Steam Ablation): A minimally invasive procedure that uses water vapour (steam) to destroy excess prostate tissue, which is then naturally absorbed by the
- HoLEP (Holmium Laser Enucleation): A highly effective laser treatment often used for larger prostates, essentially cutting out the obstructing lump via telescope and breaking it into little pieces for extraction.
- TURP (Transurethral Resection of the Prostate): The traditional “gold standard” where excess tissue is removed by cutting away chips using an electrical current, though this is now often superseded by newer technologies using different energy forms.
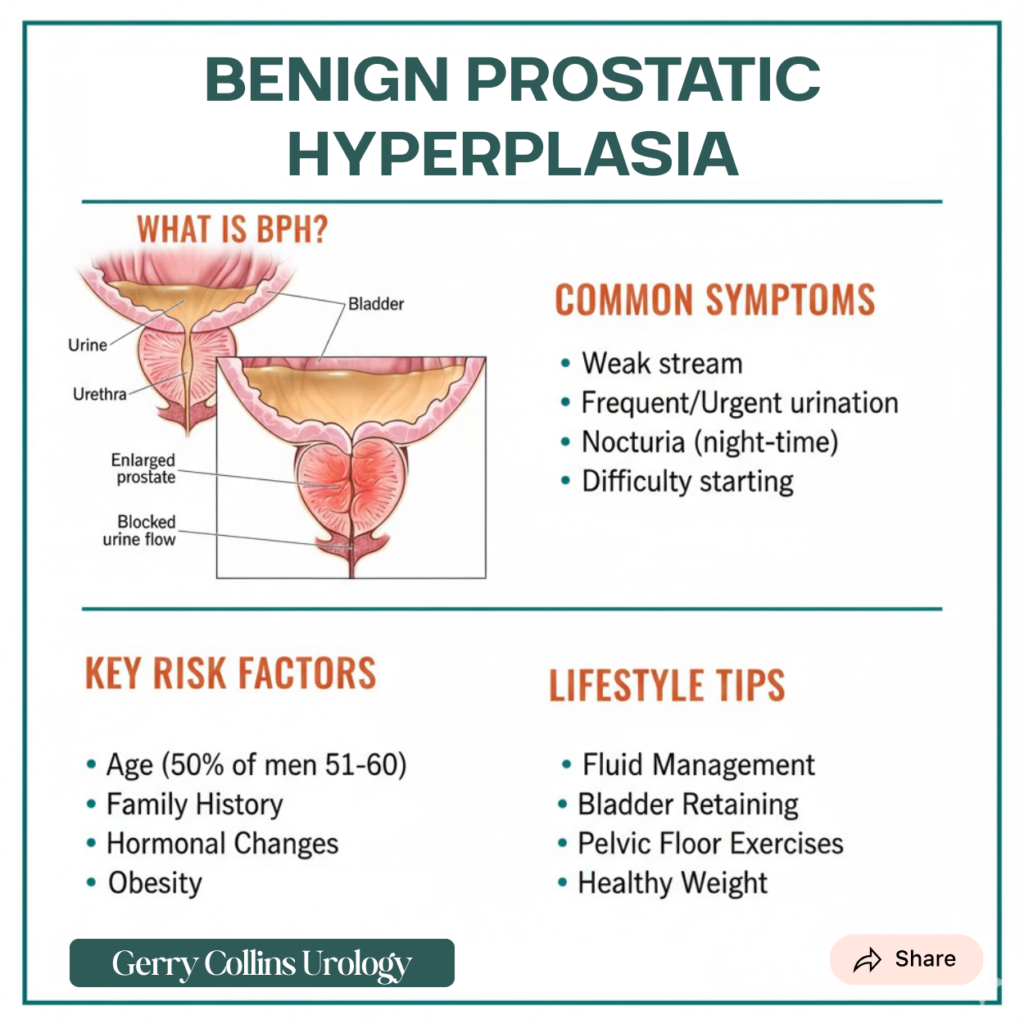
The Prevention: Lifestyle tips to do at home
While you cannot stop the natural growth of the prostate, you can manage the symptoms and support bladder health through proactive habits:
- Fluid Management: Reduce fluid intake in the late evening, particularly caffeine and alcohol, to minimise trips to the bathroom at night.
- Bladder Retraining: Try to gradually increase the time between bathroom visits to strengthen the bladder’s capacity.
- Double Voiding: After you finish urinating, wait a few moments and try again to ensure the bladder is as empty as possible.
- Pelvic Floor Exercises: Strengthening the muscles around the bladder can improve control and reduce urgency or leaking.
Maintain a Healthy Weight: A diet rich in vegetables and healthy fats can help regulate the hormones associated with prostate growth.
FAQs
No. BPH is a benign (non-cancerous) condition. While the symptoms of BPH and prostate cancer can sometimes overlap, BPH does not lead to cancer. However, because both are more common as men age, Mr Collins recommends regular assessment to ensure an accurate diagnosis.
Traditional surgeries like TURP carry a risk of “retrograde ejaculation.” However, modern, minimally invasive treatments like UroLift and Rezum are specifically designed to preserve sexual and ejaculatory function though may be slightly less effective in dealing with the obstruction. This is a key part of the consultation process with Mr. Collins.
Yes, but it must be interpreted with “Clinical Discernment.” An enlarged prostate produces more PSA (Prostate-Specific Antigen), which can lead to a raised result even without cancer. Mr. Collins uses PSA density (adjusting the result for the size of your prostate) to get a clearer picture of your health.
If your symptoms are mild and not bothering you, “watchful waiting” is a valid pathway. However, if you are straining to pee or feeling incomplete emptying, it is better to act early to prevent long-term damage to the bladder muscle.




